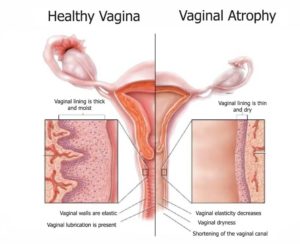
[simple_tooltip content=’The period preceding menopause. Typically starts around 40 years old and lasts 8-10 years.’]Perimenopausal[/simple_tooltip] and [simple_tooltip content=’The period following menopause.’]postmenopausal[/simple_tooltip] women may sometimes experience vaginal discomforts such as dryness, itching, burning, painful intercourse, and troubling urinary symptoms. In medical terms, this can be sometimes diagnosed as vaginal atrophy (VA). It can be described as the thinning, drying and inflammation of the vaginal walls caused by the normal decrease in estrogen levels as women grow older. Below is a diagram of the vaginal lining, showing the difference between healthy tissue and VA.
 Over-the-Counter Lotions and Gels
Over-the-Counter Lotions and Gels
There are some treatment options both prescription and non-prescription for these symptoms and conditions. Non-hormonal options are the first line agents commonly used for symptom relief. Current treatments in this category include water-based lubricants, vaginal moisturizing bases, and topical vitamin E. Water-based lubricants, such as Good Clean Love’s Almost Naked or Emerita’s Personal Moisturizer, provide short-term relief to patients during intercourse but have minimal long-term efficacy for symptom relief. Vmagic is a non-prescription oil-based option that we recommend for women needing a longer-term vaginal moisturizer.
Hormone-Based Medications
As mentioned, there are some prescription medications that can also bring some relief from symptoms. In the prescription world, there are both hormone-based and non-hormone-based option, we will discuss the hormone-based options first. Some of the more common hormones used to treat VA include DHEA, Estradiol, and Estriol. Each of these agents can be used to provide a hormonal balance; in essence, to help replace hormones that may have been more abundant before peri or post menopause. Essentially, they help to rejuvenate vaginal tissue and lining which helps decrease symptoms previously discussed. Some of these treatment options are made by large pharmaceutical manufacturers and are available any retail pharmacy.
Custom prescription options are available at a compounding pharmacy that specializes in hormone replacement therapy. It is important to note that post-menopausal women that still have a uterus must also balance an estrogen-based replacement by adding progesterone as well. Your medical provider or one of our pharmacists can explain more about the importance of protecting the uterine lining with progesterone in these circumstances.
Non-Hormone-Based Medications
There are also some prescription non-hormonal options for women who cannot use hormones due to a history of estrogen-based cancers. Women with a personal or familial history of estrogen-based cancers such as breast, ovarian, and endometrial cancers, should not use estrogen or DHEA based products because they can increase the risk of developing these hormone-fueled cancers.
A promising solution for women unable to use hormone replacement therapy is a vaginal cream or suppository formulation of the combination of a moisturizing base, vitamin A, and vitamin E. Vitamin A and vitamin E help to prevent the degradation of the vaginal tissue. They have antioxidant and anti-inflammatory properties that promote healing. Vaginal moisturizing bases help to store large amounts of water in the vaginal tissues, thus preventing dryness, itchiness, and burning, thus decreasing discomfort. A 2016 study from the International Journal of Community Based Nursing and Midwifery evaluated the effectiveness of a moisturizing base versus Premarin® (a commonly used form of estrogen) for the treatment of vaginal atrophy. 56 women were split into two groups, with half receiving Premarin® and the other half receiving a moisturizing base. Each group intravaginally applied an applicator of the drug as directed at bedtime for a period of 8 weeks. Though both treatments were efficacious in treating symptoms, the group using the moisturizing base produced the best results. The moisturizing base provided more relief of vaginal dryness, urinary incontinence, itching, and painful intercourse than Premarin®. It was concluded that the use of a moisturizing base is a suitable alternative treatment for vaginal atrophy symptoms.
The combination of a moisturizing base, vitamin A, and vitamin E has been shown to enhance the benefits of each product and provide patients with optimal symptom relief. A 2008 study from the European Review for Medical and Pharmacological Sciences assessed the efficacy of a vaginal suppository containing a combination of a moisturizing base, vitamin A and vitamin E. Participants included 126 women aged 44 to 64 experiencing menopause for at least one year, with vaginal dryness or other related symptoms. Participants were given one vaginal suppository before bed for 2 weeks, then one suppository every other night before bed for 2 weeks. After four weeks of treatment, 89.6% of patients reported an improvement in their symptoms. This study concluded that the combination of a moisturizing base, vitamin A and vitamin E has great potential for slowing down the natural process of aging of the vaginal tissues, and for increasing their natural hydration.
These non-hormonal based options are available only at a compounding pharmacy. The pharmacists at Coastal Pharmacy & Wellness have seen firsthand the positive impact that this non-hormonal combination has had on patients (see the testimonial from one of those patients below).
At the age of 58, I am 14 years post-menopausal. So issues of vaginal dryness have plagued me, as have recurring urinary tract infections. I spent some time using the Estring and liked it but eventually, I experienced burning from this. I switched to a compounded estrogen cream. Then I developed breast cancer. I am not blaming the treatment. It just happens to (some) women. My cancer was triple negative with 5 % estrogen positivity. I am taking an aromatase inhibitor for one year now. I have stayed on the estrogen cream until I felt like it was no longer working. I developed UTIs again and burning. (My doctor) recommended the natural compounded vaginal suppository and I have been on this for about three months. I am very happy with it. I am no longer experiencing burning or infections. It’s easy and comfortable and (my doctor) said there is nothing in the compound that will cause any harm even if I stay on it for a long time. It has been a blessing to me.
Thank you for providing me with a perfect solution.
Judy B
As further research emerges, we hope to see more patients benefit from this compounded formulation.
References:
- Vaginal Atrophy. Lexicomp Online, Hudson, Ohio: Wolters Kluwer Clinical Drug Information, Inc.; July 31, 2018; Accessed September 26, 2018.
- DeReese A. Treatment options for vaginal atrophy: what do the newer studies show? PCCA Apothagram. January 2011.
- Constantino D, Guaraldi C. Effectiveness and safety of vaginal suppositories for the treatment of the vaginal atrophy in postmenopausal women: an open, non-controlled clinical trial. Eur Rev Med Pharmacol Sci. 2008;12(6):411-416.
- Jokar A, Davari T, Asadi N, et al. Comparison of the hyaluronic acid vaginal cream and conjugated estrogen used in treatment of vaginal atrophy of menopause women: a randomized controlled clinical trial. 2016:4(1):69-78.