The Centers for Disease Control reports that 1 in 4 deaths in the United States can be attributed to cardiovascular disease (CVD). Given that sobering statistic, it’s reasonable to ask why this is the case despite CVD being a common concern for over 80 years.
Numerous explanations have been put forth to explain this trend. By far, the most enduring idea was introduced in the 1940s by physiologist Ancel Keys and is commonly known as the “lipid hypothesis.” Keys suggested that there was a causative link between dietary intake of cholesterol and saturated fat to adverse cardiovascular outcomes.
It is true that saturated fat in the diet prompts the production of cholesterol and that cholesterol is found in arterial plaque. That said, the nature of lipids produced through consuming saturated fat does not increase cardiovascular risk factors per se. This is due to the size and buoyancy of the cholesterol produced from saturated fat, which makes it less likely to adhere to the arterial lining.
By contrast, consumption of simple starches and sugars (which began to accelerate in the 1950s) directly provokes the production of smaller, denser cholesterol or sdLDL-c. This version of cholesterol can embed itself into arterial tissue, contributing to the plaque formation associated with cardiovascular disease.
While sdLDL-c is clearly a lipid of concern, it is perhaps more likely to create disease under conditions of chronic disruption of the cells that line blood vessel walls. This disruption compromises arterial lining function through repeated exposure to elevated levels of homocysteine thiolactone (HTL).
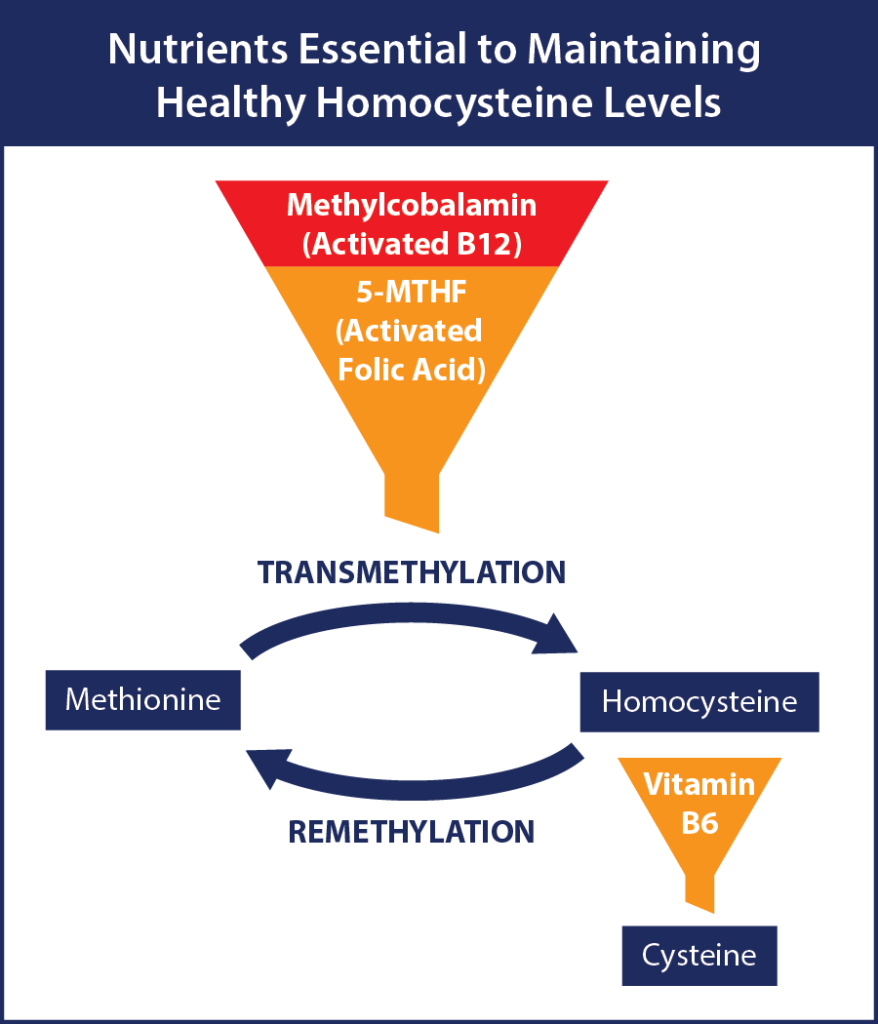
Under ideal conditions, homocysteine is produced and converted to other essential chemistry. It is then recycled back to its parent amino acid methionine or converted to cysteine, a conditionally essential amino acid. This constant chemical recycling prevents HTL build-up and helps to maintain optimal blood chemistry.
The process fails when certain nutrients are not present to facilitate the conversion. As levels of unmetabolized homocysteine increase, an inflammatory response is generated in the arterial linings, sdLDL-c is oxidized, and the production of nitric oxide is suppressed. Over time, these influences can lead to degradation of arterial linings, the formation of fatty plaques (orthogenesis), and hypertension.
In addition to cardiovascular issues, elevated HTL is associated with dementia and other neurological disorders, osteoporosis, cancer, and many other conditions.
Other factors contributing to elevated HTL include cigarette smoking and high alcohol and coffee consumption.
Some medications, including cholestyramine, metformin, and proton pump inhibitors, may also increase homocysteine.
A Nutritional Approach to Managing Homocysteine
Apart from sugars and starches, high protein diets (greater than 100 grams per day) and protein from red meat, in particular, may also contribute to elevated homocysteine. Typical adult protein requirements are 50 to 60 grams per day.
Optimal levels of homocysteine are less than ten micromoles/Liter(µmol/L), while numbers over fifteen µmol/L are considered high.
The primary nutrients necessary to manage homocysteine:
- 5-methyltetrahydrofolate or 5-MTHF (the active form of folic acid)
- Methylcobalamin (an active form of vitamin B12)
- Pyridoxal-5-phosphate or P-5-P (the active form of vitamin B6)
While it is possible to obtain these vitamins from dietary sources, it is unlikely that we can achieve rapid suppression of elevated homocysteine with diet alone. Care should be taken to choose the active forms due to possible difficulty converting precursor nutrients (i.e. folic acid) to their active state.
Assuming therapeutic interventions have achieved the goal of lowering homocysteine in the short term, a whole food diet may help to maintain levels within an optimal range. This type of diet includes leafy greens, colorful fruits and vegetables, lean protein, and healthful fats (including fish, coconut, and olive oils).
A Note Regarding the Effects of Exercise on Elevated Homocysteine
A recent meta-analysis of studies investigating how physical activity might influence homocysteine levels showed that various forms of aerobic exercises had an essentially neutral effect. However, strength training was noted to lower homocysteine, at least in the short term. It seems prudent to pursue a variety of physical activities, as their overall health benefits are well-established.